The Skin Side Effects Of Organ Transplants
A Common Organ Transplant – The Kidneys
Organ transplantation is usually the best option for a person with a serious organ disease. It reduces the chances of death and illness and can dramatically improve a patients wellbeing. However, despite becoming increasingly common, transplants are not without their risks.
Recent studies now establish a clear link between transplants and skin diseases. Although in most cases, these skin diseases are far a better option to the alternative without a transplant, some skin diseases can be serious. Complications can range from skin cancer to more typical problems such as eczema. Here we look into the most common skin diseases and what causes them.
How do Skin Problems Occur with Transplants?
As it stands, transplants may cause skin diseases through 2 different methods:
- The transplant itself transfers or causes an infection
- The immunosuppressive drugs cause a flare up post operation
The type of skin disease that occurs, can usually determine whether it was due to an infection or the immunosuppressive treatment after an operation.
What is Immunosuppressive Treatment?
Firstly, what is this anyway? Immunosuppressive treatment is an integral part of organ transplants. For a transplant to be successful in the long term it depends on preventing organ rejection. Assuring the body does not reject the organ is vital to recovery.
To prevent rejection, many different drugs are used to reduce the persons cellular immune responsiveness. In simple terms, the drugs are there to tell our body to calm down and not aggressively attack the new organ. Although these drugs are effective and in many cases absolutely necessary, they can come with side effects.
Skin diseases caused by organ transplants
To begin, let’s start with the skin diseases most commonly caused by the transplant itself (not the immunosuppressive treatment). Usually these diseases are viral and fungal. You can click the link on each disease to learn more.
![Herpes Zoster (Culebrilla) (20) piel [ICD-10 B02]](https://firstderm.com/wp-content/uploads/Herpes-Zoster-Culebrilla-20-piel-ICD-10-B02.jpg)
An Example of Herpes Zoster
In most cases these diseases appear within 5 years of the transplant. The majority of studies analyse Renal transplants since these are most popular but the results are similar for all transplants.
Viral warts are also the most common of all infections with 15% of all transplants in the study reporting an occurrence. In fact, this number increased to 50% of cases within a 5 year period. The reason this is particularly concerning is due to the effect on the patients wellbeing and, importantly, the risk of developing into skin cancer.
Skin Cancers
![Basalcellscancer (basaliom) (16) hud [ICD-10 C44.91]](https://firstderm.com/wp-content/uploads/Basalcellscancer-basaliom-16-hud-ICD-10-C44.91.jpg)
An Example of Basal Cell Carcinoma
Unfortunately, there is also an increased risk of skin cancer with organ transplants. The most commonly found skin cancers are:
- Basal Cell Carcinoma
- Bowen’s Disease
- Extrammary Paget’s Disease
- Squamous Cell Carcinoma
As a general rule, the research finds that skin infections tend to develop early after the transplant whereas skin cancers form later. This is an important factor when monitoring a patient post operation. As mentioned earlier, this could be due to the risk of warts developing into cancers such as Squamous Cell Carcinoma.
What Skin Diseases are caused by Immunosuppressive treatment?
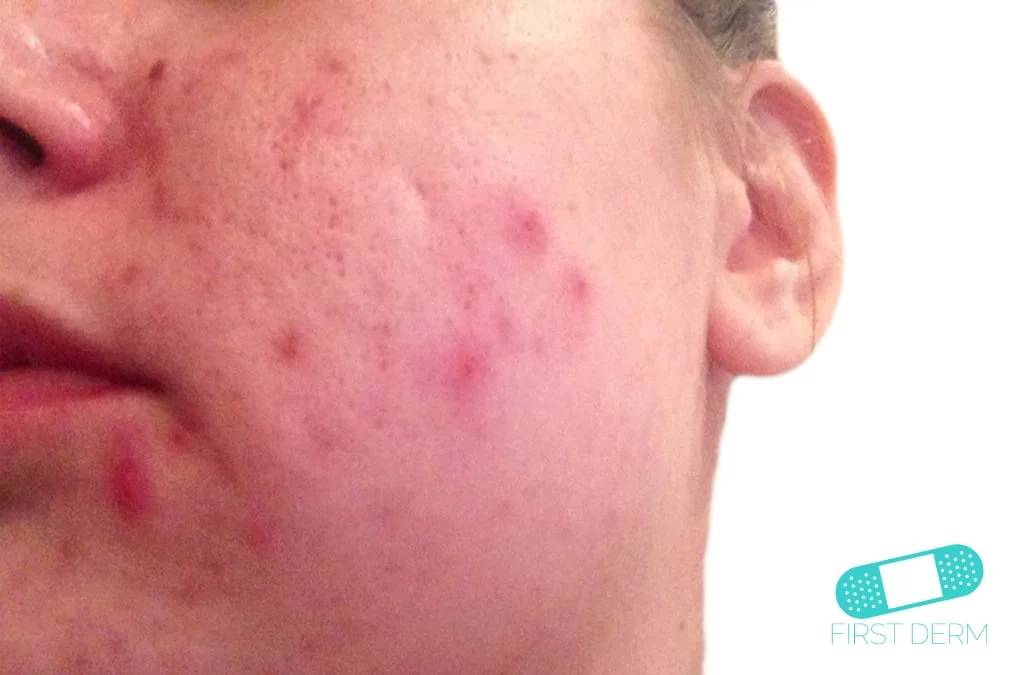
An example of Acne
Immunosuppressive treatment involves a variety of drugs designed to reduce the bodies immune response to the transplant. These drugs are typically a form of steroid such as prednisone and can invoke skin diseases such as:
As well as these 2 skin diseases there are a range of other diseases that may or may not be attributed to the drug treatment.
These include:
- Eczema
- Hair Loss
- Seborrheic Keratosis
Although classed as ‘other’ over 12% of cases reported were Eczema which is very high. The reason for labelling as other is due to the many factors that cause skin diseases such as eczema. Like hair loss, the cause is very difficult to determine. It is, therefore most likely a combination of drug treatment and the stress of having an operation but there could be many other factors.
Treatment
In almost all cases, it is about managing the patient and monitoring their health. Doctors advice is to stay out of the sun where possible to reduce the risk of skin cancer. There is also a strong argument for monitoring patients regularly within the first 5 years. It is in this period that most skin complications are likely to occur.
Doctors are also now considering a HPV vaccine before treatment but more research is needed to determine the optimal vaccine type.
Consult a Dermatologist
If you notice something suspect, be it a mole, rash or mark we always suggest speaking to your GP. They should be able to check the problem and recommend you to a dermatologist if needed. Alternatively, we have board-certified dermatologists on hand to deal with any concern. Simply send in an image and we’ll do the rest.
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.

