Athlete’s foot – Tinea Pedis – Diagnosis, Symptoms and Treatment
Walk Away from Athlete’s Foot
Athlete’s foot. The contagious—and annoying—fungus that thrives in the warm, moist environment of your toes, causing itching, redness, and cracking. Your feet are magnets for fungal infections. And these fungi can lurk almost anywhere.
Most people are aware the fungus grows on the warm, damp surfaces found in public spaces— gyms, locker rooms, showers, and swimming pools – and very common in hiking. Walk barefoot and it will likely end up on your feet. Wearing shoes on wet, germ-filled surfaces will decrease your chances of contracting the infection. A wide variety of fungi can cause Athlete’s foot. All belong to a group called dermatophytes. These fungi feed on keratin, a protein found in hair, nails, and skin.
Protecting your feet from fungi doesn’t have to be hard, though. You just need to know where to start. Here are four lesser-known causes of athlete’s foot, and your best defenses against them.
Contact a dermatologist about your skin conditions.
A typical user question
Question
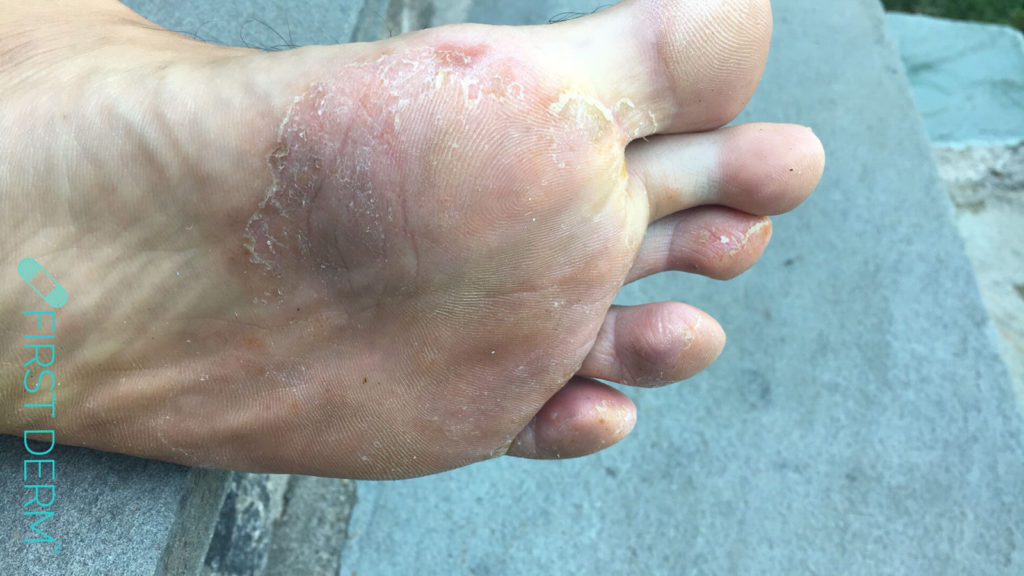
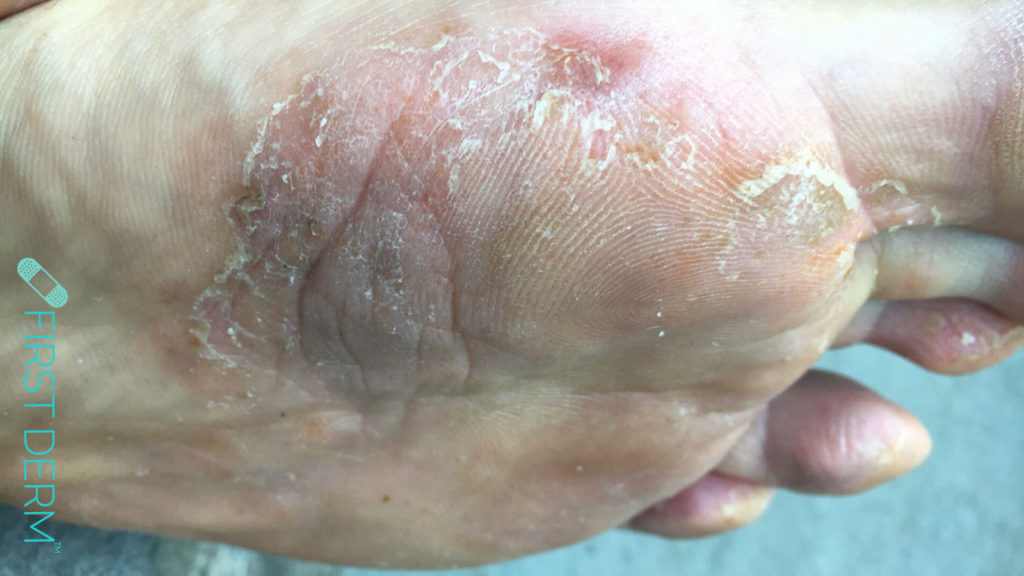
I am a 43 year old man. I have had an issue with my foot the last few weeks. Itchy, flaky, sometimes blisters also in between the toes. Attached are two pictures
Answer
Thank you for sending your case. Based on the information and images of your foot this appears to be TINEA PEDIS. Athlete’s foot is a fungal infection between toes caused by warm, moist, tight conditions around feet and toes. You can treat this with over-the-counter anti-fungal preparations with the addition of hydrocortisone. Preventive measures include good feet hygiene, changing socks frequently and keeping the area between the toes dry. Also, I suggest purchasing “Lotrimin Ultra Athlete’s Foot Spray” over-the-counter available at CVS Pharmacy. Apply twice daily for 2 weeks. If despite using the above measures, your condition does not improve in 10 to 14 days, you should see a dermatologist for prescription treatment. Your dermatologist can prescribe topical and or oral anti fungal medications to treat the condition.
Pets
Dogs and cats shed tiny specks of skin called dander. Fungi can easily travel on your pet’s dander throughout your home. As you walk barefoot through your rooms, the dander can attach to your soles and cause an infection. To keep your feet fungi-free at home, bathe your pets with an anti-dander shampoo to minimize flaxes. Vacuum your floors often and wear slippers in the house.
Tight Shoes
Toes trap in more moisture when they’re squeezed together. There are most likely fungi already between your toes, and the moisture gives it the environment it needs to grow. When you’re shopping for shoes, make sure you can comfortably wiggle your toes before you buy them.
Socks
Your choice of socks can also increase your risk of infection. Cotton acts like a sponge. It stays wet when you sweat. But synthetic materials wick away wetness. If you’re prone to sweating, use a roll-on antiperspirant on the bottom of your feet to help keep them dry.
Not wearing socks can also leave you susceptible to athlete’s foot. Without socks, your shoe rubs off dead skin cells from your feet. Fungi can live on the cells and remain inside your shoes until the next time you slip them on. Spray the inside of your shoes with an antifungal spray to kill any fungus that may be lurking there.
Contact a dermatologist about your skin conditions.
Your Own Skin
Open wounds make it easy for fungi to live on your foot. But it’s not just cuts that make you vulnerable. Dry, cracked heels are also easy targets. Moisturize heels and treat blisters or cuts with an antifungal cream. If you have a wound, try to limit the amount of time you’re in bare feet and avoid moist surfaces where germs are found, such as locker rooms, pools decks, and shower floors.
When to contact a dermatologist
If you do happen to contract Athlete’s foot, you can try over-the counter creams or sprays for at least two weeks. But if after that time, you don’t see improvement, it’s time to contact a dermatologist. He or she can prescribe topical creams. Check in with a doctor even sooner if you have fever, swelling, or itching that keeps you up at night.
If your infection spreads to the nails, it can be treated with special prescription nail preparations, but oral medication is often more effective. Unfortunately, Athlete’s foot is not something that goes away easily. Even with daily treatment, it may take about two to six months to clear up.
Contact a dermatologist about your skin conditions.
Fit these preventative measures into your daily routine.
- Always clean and dry your feet immediately after showering.
- Put on your shoes as soon as you get out of the shower. The risk of infection still exists outside of a shower.
- Apply lotion, cream, or oils daily. The more moisturized your feet are, the less likely you are to have cracks in the skin, which is how the fungi causes inflammation.
- At home, sanitize shower bases with a diluted bleach solution. This kills spores of fungi.
- There is always the risk of fungal infections. But if you maintain proper foot hygiene, the risks are actually very low.
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.