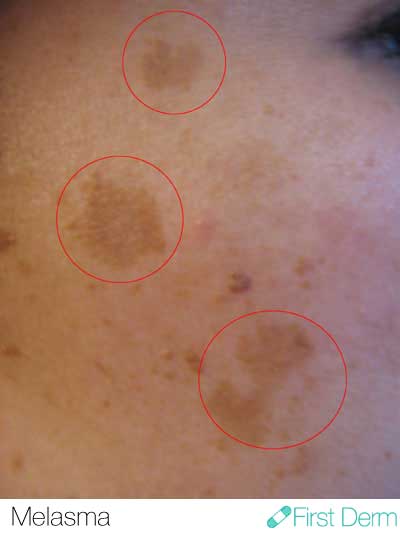
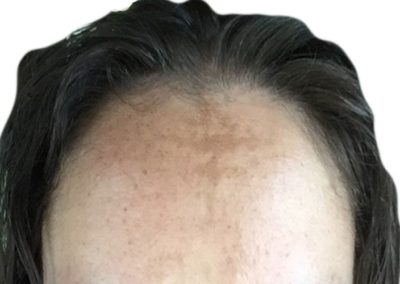
Melasma (Chloasma)
Medically reviewed by The Dermatologists and written by Dr. Alexander Börve
Common Very common in people older than 30 who have been exposed to sun
- Often self-diagnosable
- Symptoms: Brown or gray-brown patches, darkening of existing moles
- Color: Typically brown or gray-brown
- Location: Anywhere on the face most exposed to the sun
- Treatment: No treatment necessary; bleaching cream, pigment laser
Related Blog Posts: Sunscreen decoded: Is higher SPF better? Sunburns: It’s time to get real When Your Child Says NO to Sunscreen The Best Sunscreen Is One You’ll Use
Melasma, previously known as chloasma, presents as gray-brown, irregularly shaped, persistent spots on the face. This is also a ‘photoaging’ condition, which means sun damage is causing your skin to age prematurely.
Melanocytes are important to produce the pigment ‘melanin’ which gives the color to your skin. In this condition, melanocytes get over active and produce copious amounts of melanin and gives the pigmented appearance. There are several factors that trigger melanocytes to cause chloasma.
Try our FREE dermatology search engine and get peace of mind within a second
What causes Melasma (Chloasma Faciei)?
This skin condition is most common on the face of young women after tanning. This is because the ultraviolet (UV) light stimulates melanocytes (dark pigment imparting cells) in the skin. Sun exposure can make melasma return after fading.
The condition could also be triggered by hormones caused by contraceptive pills, hormone replacement medicine or pregnancy. Studies show 30% of women in child bearing age are affected by melasma.3 This is why many people call it the pregnancy mask. Hormones that trigger chloasma faciei include estrogen and progesterone.
Women are more likely to get melasma than men. People with skin of color are more prone to melasma because they have more active melanocytes than those with light skin. This means that those of Latin/Hispanic, North African, African-American, Asian, Indian, Middle Eastern, and Mediterranean descent are more likely to get melasma.
In addition, it has a strong genetic predisposition. This means people who have a blood relative who had melasma are much more likely to get melasma. Thyroid medication is another thing that makes you prone to get melasma.
Symptoms
Melasma manifests itself as brown, grayish brown or beige-brown patches. These patches won’t cause any symptoms, and will be distributed symmetrically on your face. Most people get it on their cheeks, bridge of their nose, forehead, chin, and above their upper lip. It also can appear on other parts of the body that get lots of sun, such as the forearms and neck.
Some may experience darkening of existing freckles, areolas (nipples), and moles or a dark line down the center of the abdomen, which is known as Linea nigra. Almost constant worsening of these irregular bordered dark patches is another unique feature of this condition.
Melasma is diagnosed by these symptoms, and the diagnosis might be helped with the history of exposure to triggering factors mentioned above. There is a method called Wood’s lamp examination where the dark patches are examined under the light of this specific lamp, in order to determine if the melasma is in the epidermis; the outermost layer of skin, or if it is in the dermis as well; the layer just deep to the epidermis. This is important because in the former case, it responds better to treatment with creams and other topical medication.
Try our FREE dermatology search engine and get peace of mind within a second
What can I do?
Even though there is no treatment for melasma, it may fade on its own. This often happens when the trigger is pregnancy or birth control pills. When the woman delivers the baby or stops taking the birth control pills, melasma may fade.
You can also protect the affected areas from the sun. You can wear sunscreen every and reapply it every 2 hours to achieve so. This is also important to prevent relapse of melasma after it fades away spontaneously or with treatment. Some dermatologists also recommend wearing a wide-brimmed hat when you are outside, as sunscreen alone may not give you all the protection you need.
When you are choosing the sunscreen, there are several things to consider. Especially, new evidence proves not only UV light, but also short wave length visible light rays (blue-violet) have the ability to cause melasma by inducing hyperpigmentation.5 So, it is important to go for a sunscreen that contains iron oxide, which provides protection against the latter type of waves.
Some studies show that folate deficiency can be related to hyperpigmentation. Therefore, you can try including green leafy vegetables, oranges, whole-wheat bread, and whole-grain cereal to your diet. You should also stop using skin care products that irritate the skin, as it may worsen melasma.
Should I seek medical care?
If self-treatment does not improve your situation or causes skin irritation and darkening, you should seek help from a dermatologist.
Treatment
Management of melasma is a very challenging task because of the inconsistent treatment results. Also, there is the added burden of almost certain reappearance of the condition. Therefore, there is no treatment that can cure melasma completely to the date. The reason might be the fact that most of the current treatment options focus on melanocytes and only try to fix the hyperpigmentation. But new information show melasma is more of a photoaging condition, which means there are other cells and factors contributing to dark patches you get in melasma. If we can try to treat all those factors as well, more effective treatment methods will surely emerge.
Treatment options can be categorized into 3 groups, according to the method of action.
- Topical skin lightning agents – focus on melanocytes and reduce melanin production
- Chemical peels – remove the extra melanin from the skin surface
- Laser and other light-based therapies – remove the excessively pigmented areas from the skin
There are various methods to reduce the symptoms. Meticulous use of high SPF sunscreen, topical retinoids, azelaic acid, bleaching cream, or a pigment laser under dermatologist supervision can help reduce pigmentation. It may take a few months of treatment to see improvement.
Out of all these options, gold standard is considered to be topical bleaching agents.3 By reducing the melanin production, these skin lightning agents are capable of reducing the color in the hyperpigmented are of your skin. For example, a topical agent called ‘Kligman’s formula’ containing a mixture of corticosteroid, retinoic acid and hydroquinone is proven to be very effective mean of treatment.
Chemical peels are also an option to consider. In this method, deposited excess melanin is removed from the skin surface. Most of the time chemical peels are done simultaneously with topical agents. However, this method includes many complications and side effects like post -inflammation hyperpigmentation (PIH) where you get darkened patches of skin following inflammation. Light based therapies come last, if all else fails. The outcome of treatment with lasers and topical creams have been studied and documented. This shows the topical creams like Klingman formula are more effective than copper bromide lasers.4
If you’re pregnant or breastfeeding: Don’t use peels, bleaches or other chemically based lightening treatments, since they can potentially penetrate the skin. When it comes to the timing of the treatment, the sooner you start treatment the better. If you have had it for a long time, the therapy is less likely to give you quick results. However, this changes if you are pregnant. One reason is the potential harm to the baby, and another is melasma often fades away on its own after you give birth. So, it is best to wait until then before going for a treatment option right away.
Melasma, formerly known as chloasma faciei is a mostly harmless hyperpigmentation condition where you get dark patches of your skin. However, melasma has a negative impact on one’s social life and causes emotional distress to patients. Studies have shown the reduced quality of life patients experience because of this condition.6 So, do not hesitate to contact your dermatologist if you are bothered by the cosmetic inconvenience these dark spots are causing, even though they are otherwise harmless.
Source:
- American Academy of Dermatology. Melasma. Available at: https://www.aad.org/public/diseases/color-problems/melasma
- What to Expect. Chloasma (Mask of Pregnancy). Available at: http://www.whattoexpect.com/pregnancy/symptoms-and-solutions/chloasma.aspx
- Passeron, T., & Picardo, M. (2018). Melasma, a photoaging disorder. Pigment Cell & Melanoma Research, 31(4), 461–465. https://doi.org/10.1111/PCMR.12684
- Ghorbel, H. H., Boukari, F., Fontas, E., Montaudié, H., Bahadoran, P., Lacour, J. P., & Passeron, T. (2015). Copper Bromide Laser vs Triple-Combination Cream for the Treatment of Melasma: A Randomized Clinical Trial. JAMA Dermatology, 151(7), 791–792. https://doi.org/10.1001/JAMADERMATOL.2014.5580
- Duteil, L., Cardot-Leccia, N., Queille-Roussel, C., Maubert, Y., Harmelin, Y., Boukari, F., Ambrosetti, D., Lacour, J. P., & Passeron, T. (2014). Differences in visible light-induced pigmentation according to wavelengths: a clinical and histological study in comparison with UVB exposure. Pigment Cell & Melanoma Research, 27(5), 822–826. https://doi.org/10.1111/PCMR.12273
- Zhu Y, Zeng X, Ying J, Cai Y, Qiu Y, Xiang W. Evaluating the quality of life among melasma patients using the MELASQoL scale: A systematic review and meta-analysis. PLoS One. 2022 Jan 27;17(1):e0262833. doi: 10.1371/journal.pone.0262833. PMID: 35085327; PMCID: PMC8794204.
Ask a Dermatologist Now
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.
![Melasma (Chloasma) (08) cheek woman [ICD-10 L81.1]](https://www.firstderm.com/wp-content/uploads/Melasma-Chloasma-08-cheek-woman-ICD-10-L81.1-e1592824542826-400x284.jpg)
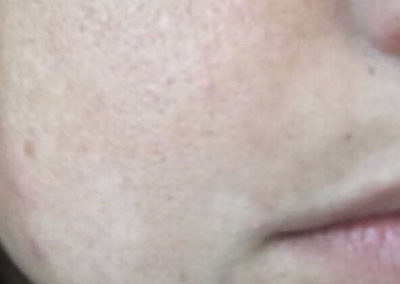
![Melasma (Chloasma) (10) cheek woman [ICD-10 L81.1]](https://www.firstderm.com/wp-content/uploads/Melasma-Chloasma-10-cheek-woman-ICD-10-L81.1-e1592824596216-400x284.jpg)