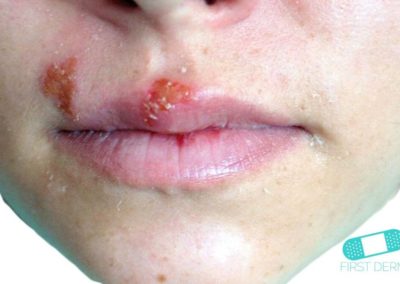
Oral Herpes Simplex (Cold sores)
Medically reviewed by The Dermatologists and written by Dr. Alexander Börve
Common Very. 50% of the US population
- Requires medical diagnosis
- Symptoms: Blisters appear singly or in a group
- Color: Typically red, but can vary
- Location: Around the mouth
- Treatment: No known cure, can be relieved by antiviral creams
Herpes is a common skin disease that can be categorized into two categories: HSV-1 and HSV-2. Both types of herpes may present with symptoms of blisters or sores in the affected region. Some individuals, for instance, are unaware that they have the disease because their symptoms are so minor. Others, however, may have many outbreaks per year. HSV-1 and HSV-2 are most commonly associated with outbreaks around mouth and genital area, respectively – although either type may be found in either location. Herpes simplex can also infect fingers and the eyes.
Oral herpes, also known as labial herpes, is usually caused by HSV-1, which is found in saliva and is transmitted mainly through mouth-to-mouth contact. Transmission of the virus can also occur through direct contact with the sores or secretions and sharing utensils or lip products. Through oral sex, HSV-1 can be transmitted to genital areas and cause genital herpes, but it is rare that HSV-2 infects the mouth.
Once infected with oral herpes, you have some immunity against genital herpes, even though the different virus types prevent them from having complete immunity against each other.
Symptoms
Herpes blisters (also known as fever blisters or cold sores) appear as one or more blisters in a group around the affected region. The sores are typically inflamed and painful, and over the course of the outbreak, they may leak clear fluid and leave a scab. There is a lot of variability in terms of the duration, appearance, and repeating herpes outbreaks. The most typical additional symptom during the initial outbreak may include fever or fatigue.
Oral herpes is most commonly seen as cold sores on the lips or the skin around the mouth, with clusters of small fluid-filled blisters that often hurts. You can also get the same sores inside the mouth on the tongue, gums or palate. The skin around the blisters and the mucous membranes inside the mouth tend to blush or get swollen with HSV-1 infection. It often hurts and is already swollen one or two days before the blisters are formed. Oral herpes usually does not give any scars.
When you get the disease for the first time, it is called ‘primary infection’. Primary infection is often symptomless, or give rise to an infection in the pharynx, which is the uppermost part both the respiratory and alimentary tracts share. So, it is not easy to differentiate this from an upper airway infection. However, the primary infection is most of the time preceded by other systemic symptoms like headache, fever, a general feeling of discomfort, nausea or vomiting. Ulcers or vesicles appear in the mouth one to two days after that, which is called ‘acute marginal gingivitis’. So, these can be used to identify oral herpes from other ulcerative diseases of the mouth. Young children who get herpes for the first time can get strep throat-like symptoms, sometimes without blisters on the lips.
Get peace of mind and get a Lab Test for Herpes today
However, the herpes virus does not disappear from the body after an outbreak. From the skin the virus moves to nerve cells next to the spinal cord where it lies dormant. It can be activated again and give cold sores again, especially when you are sick with the flu or pneumonia, expose your skin to strong sunlight, stressed or menstruating. When oral herpes recurs, the first symptom is often an uncomfortable tingling or throbbing sensation in the skin around the mouth.
Most common herpes virus type that recurs is recurrent herpes labialis (RHL). The symptoms typically appear on the border of the lips where the mucus membrane and the skin meet, which is known as vermillion boarder. This recurrence is more common in patients receiving cancer chemotherapy, immunosuppressive drugs or AIDS patients. In such immunosuppressed people, oral herpes lesions can lead to disseminated generalized infection, where the herpes sores appear on the face and other parts of the skin that are normally not affected. Several studies have shown the successful treatment of recurrent herpes infection with topical treatments, but to suppress the virus chronically, systemic treatment is required.5
How does it spread?
Out of all infections of the mouth, herpes virus is the most common.3 Oral herpes is spread through saliva. If you come to direct or indirect contact with an infected person’s saliva, you are at a risk of getting the disease. Also, you can get oral herpes during oral sex with a person infected with genital herpes. More alarming fact is, the disease spreads not only during ‘herpes outbreaks’ when there are visible symptoms, but also in the periods where no symptoms are preset.
Your dermatologist would be able to diagnose oral herpes by assessing the blisters. The diagnosis can be confirmed by the presence of the virus in the discharge released by the blisters, or by the presence of specific antibodies produced in the body against the herpes virus. In order to do that, a small sample is collected and tests are performed, such as viral culture, viral DNA test, direct fluorescent assays and polymerase chain reaction (PCR) techniques.
From birth up to 6 months, baby gets some amount of protection through the antibodies that were produced by the mother and delivered to the fetus before birth. After 6 months, protection wears off and the risk reaches a peak at around 2-3 years.4 Regardless of that, adolescents and rarely even people over 60 years of age can also get infected with oral herpes.
Hepatic whitlow
Cold sores can spread from your mouth to fingers, causing an infection in the finger. It usually affects the tip of the finger, and give rise to painful blisters, sores, swelling and redness. This is called hepatic whitlow. The blisters can be filled with pus or clear fluid, itchy and extremely contagious.
What can I do?
If you have herpes breaking out with blisters, do not kiss others. You should also wash your hands often to avoid passing on the virus through hand contact with others. You should not share lip product, utensils or food with others. Because the herpes virus can cause a painful eye infection, you should try to avoid touching your eyes with your fingers when you have a herpes outbreak.
In order to prevent recurrent episodes of herpes outbreaks, you should protect your skin from factors that trigger it. You can apply sunblock or lip balms when going out to prevent the assault from the sun. Moisturizers will help prevent your skin from drying out.
Should I seek medical care?
It is rare that wounds become infected by bacteria, where they become even more swollen and lasting. In this cases, you may need to use antibiotics.
If you have had eczema, you can be extra sensitive to cold sores. Widespread eczema can impair your immunity against herpes viruses. If you have used drugs that impair defense against infection, you may need medicine that prevents the herpes virus itself from spreading. There are both ointments or tablets that you take in the early stage of the infection.
If you are already severely immunocompromised because of a serious illness; you can also get a widespread and severe herpes infection. Other very rare complications include inflammation of the meninges, or brain. If you become very ill from a herpes infection, you should be treated in hospital.
If you are pregnant, there is a small risk that the virus may transmit to the newborn during childbirth. You should contact your doctor if you are pregnant and get a herpes outbreak for the first time or if you get an outbreak during the last trimester of pregnancy.
Get peace of mind and get a Lab Test for Herpes today
Treatment
At this time there is no known cure for either type of herpes, although there are treatments that suppress symptoms. Symptoms go away on their own in about two weeks’ time. Using medication will help you get rid of those annoying blisters faster.
There are serval antiviral creams, which will give your immune system an extra boost to fight the virus. They work best if applied before the sores develop, at the stage where warning signs of the herpes outbreak is present. Antiviral creams containing acyclovir (e.g. Zovirax) may relieve superficial symptoms. However, these creams are expensive and only reduce healing time by a few days, so you can opt for simpler methods to seek relief form pain as mentioned below.
- Apply ice or a warm washcloth on the affected are to relieve the pain.
- Rinse your mouth with cold water or salt water.
- Avoid hot drinks, spicy or citrus food, as these will cause more pain.
- Wash the blisters gently with antiseptic soap, and use a separate towel to dry the affected area to prevent further spread.
In some cases, when symptoms are severe, treatment with prescription antiviral medicine in tablet form may be required. It is not curative, but suppresses the symptoms. In these cases, treatment should start as early as possible after the first signs of disease.
And it is important to manage associated symptoms like fever by supportive care. Restoring body fluids is essential, so drink plenty of water to stay hydrated. You can use medicine to reduce fever, topical anesthetics like viscous lidocaine or a concoction called ‘magic mouthwash’ to get relief from the pain the blisters might cause. Magic mouthwash is a topical anesthetic containing liquid diphenhydramine, milk of magnesia, and Carafate.6
Since there are emerging herpes viruses that are resistant to currently used drugs, new medicine has come in to play, including valacyclovir and famciclovir. However, any of these methods are unable to eradicate the disease because none of them prevent the latency of the virus in the nervous system. Research is being conducted nowadays to find a solution to this problem, by taking the virus out completely or sealing it inside the ganglions where they survive for a long period, causing recurrent infections.7
Source:
- S. National Library of Medicine. Herpes Simplex. Available at: https://www.nlm.nih.gov/medlineplus/herpessimplex.html
- World Health Organization. Herpes simplex virus. Available at: http://www.who.int/mediacentre/factsheets/fs400/en/
- MARTIN S. GREENBERG, D., & MICHAEL GLICK, D. (2003). Burket’s Oral Medicine Diagnosis & Treatment (10th edition). BC Decker Inc.
- Stoopler, E. T. (2005). Oral herpetic infections (HSV 1-8). Dental Clinics of North America, 49(1), 15–29. https://doi.org/10.1016/J.CDEN.2004.07.005
- Balasubramaniam, R., Kuperstein, A. S., & Stoopler, E. T. (2014). Update on oral herpes virus infections. Dental Clinics of North America, 58(2), 265–280. https://doi.org/10.1016/J.CDEN.2013.12.001
- Stoopler, E. T., & Greenberg, M. S. (2003). Update on herpesvirus infections. Dental Clinics of North America, 47(3), 517–532. https://doi.org/10.1016/S0011-8532(03)00018-1
- Researchers Discover How the Cold Sore Virus, Jostled from Dormancy, Sidesteps the Immune System | NYU Langone News. (n.d.). Retrieved February 8, 2023, from https://nyulangone.org/news/researchers-discover-how-cold-sore-virus-jostled-dormancy-sidesteps-immune-system
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.