Malignant Melanoma
Medically reviewed by The Dermatologists and written by Dr. Alexander Börve
Melanoma is the deadliest form of skin cancer, as it has the potential to spread to other parts of the body. This form of cancer in skin pigment cells is often caused by the sun’s ultraviolet ray, which damage skin cells and causes the cells to divide uncontrollably.
![Malignant melanoma lesion located on the stomach, showing the characteristic dark, irregularly shaped mole associated with skin cancer Malignant Melanoma (27) stomach [ICD-10 C43.9] showing the characteristic dark, irregularly shaped mole associated with skin cancer](https://www.firstderm.com/wp-content/uploads/Malignant-Melanoma-27-skin-ICD-10-C43.9.jpg)
Malignant melanoma lesion located on the stomach, showing the characteristic dark, irregularly shaped mole associated with skin cancer
Ask a dermatologist today and get peace of mind
Symptoms of Malignant Melanoma
The disease sometimes occurs in liver spots or moles, but also may begin in normal skin. Melanoma can occur anywhere on the skin but often sits on the legs for women and on the chest and back for men.
![Malignant melanoma on the back, depicted by an irregular dark mole Malignant Melanoma (09) back [ICD-10 C43.9] depicted by an irregular dark mole](https://www.firstderm.com/wp-content/uploads/Malignant-Melanoma-09-skin-ICD-10-C43.9.jpg)
Malignant melanoma on the back, depicted by an irregular dark mole
- Superficially growing melanoma, or superficially spreading melanoma often stays thin for quite a long period of time, months to years before it begins to grow in depth.
- Knut Format melanoma or nodular melanoma grows in depth from an early stage
- Lentigo malignant melanoma, also referred to as lentigo maligna, is a more benign form of melanoma. It often appears on the face of the elderly and can grow superficially for years as a precursor of melanoma before it grows in depth.
How To Check For Melanoma?
The ABCDE rule can be used to self-check for cancerous moles: shape, border irregularity and color variability are often signs to look for.
![Close-up of a malignant melanoma on the face, marked by an uneven, darkly pigmented spot Malignant Melanoma (25) face [ICD-10 C43.9] marked by an uneven, darkly pigmented spot](https://www.firstderm.com/wp-content/uploads/Malignant-Melanoma-25-skin-ICD-10-C43.9.jpg)
Close-up of a malignant melanoma on the face, marked by an uneven, darkly pigmented spot
The ABCDE Method
The American Academy of Dermatology recommends the ABCDE method for monitoring your moles: (See images below for examples.)
- Asymmetric shape – non-cancerous moles are symmetrical
- Border irregularity – melanomas have notches or blurred edges while moles are more sharply defined
- Color variability – the color is distributed unevenly in cancerous moles
- Diameter – moles are typically smaller than ¼ inch
- Evolution – changes in size, shape, and color can indicate a melanoma
- Extra features – if a new mole is bleeding or itching, it could be cancerous
Preventing Melanoma
Melanoma prevention is an all-round project. Following these tips can lower your risk of getting melanoma:
1. Limit exposure to UV radiation. This is perhaps the most important preventative measure. Since exposure to UV radiation causes melanoma, limiting your exposure to UV radiation from the sun significantly reduces your risk of getting melanoma. Be sure to also avoid UV radiation from other sources, like tanning beds and lamps.
2. Apply sunscreen. When exposure to the sun’s UV radiation is unavoidable, be sure to apply sunscreen with SPF 15 or higher and wear protective clothes. Learn more about how to choose the right sunscreen for you.
3. Seek shade. Stay in the shade, especially between the hours of 10am and 4pm when the sun is brightest.
4. Avoid sunburns. According to the American Academy of Dermatology, one sunburn can double one’s chances of getting melanoma. For this reason, avoiding sunburns significantly reduces one’s risk of getting melanoma.
Tips to Avoid The Sun
Ultimately, you can reduce the risk of getting melanoma by avoiding sunburn. The strongest sunlight in summer is from 11am to 3pm. You get much more exposure to the sun if you are staying in an open area, such as a beach, than if you are surrounded by trees or buildings. At the beach, sun also reflects off the sand and the water, which means that you can get burned even under an umbrella or even in cloudy or hazy weather.
The best way to protect yourself during sunny days is to be in the shade as much as possible. Clothing and sun hat or cap offers good protection as well. Sunscreen is recommended as a supplement. Tanning by the sun can put you at risk of skin cancer. It is always better to let your skin get used to the sun slowly than to expose the skin for many hours of sunshine at once. New findings suggest that even excessive tanning in a solarium may increase the risk of malignant melanoma.
Ask a dermatologist today and get peace of mind
Should I seek medical care?
Any changing mole should be checked by your healthcare provider or dermatologist. If you or a health care professional finds liver spots or moles that have grown or changed in other ways, they should always be examined more closely. In many cases, it is caused by other skin changes rather than malignant melanoma, but it is important that to examine if the case indicates cancer.
Melanomas are typically brown, but may develop more colors as the melanoma grows. Itching and bleeding are often late features of melanoma – do not wait for it to bleed! Signs to look for include any new mole that grows, any mole that is changing, or any lesion on the skin that looks different.
![A distinct, darkly colored malignant melanoma lesion on the torso Malignant Melanoma (24) torso [ICD-10 C43.9]](https://www.firstderm.com/wp-content/uploads/Malignant-Melanoma-24-skin-ICD-10-C43.9.jpg)
A distinct, darkly colored malignant melanoma lesion on the torso
Ask a dermatologist today and get peace of mind
Treatment for Malignant Melanoma
The melanoma must be removed by surgery. Early treatment by surgical removal is important, as the cancer may be aggressive. Do not delay – thin melanomas can be 100% curable. The treatment results in malignant melanoma are good and most are cured after surgery. Sometimes other tests are needed, such as cell samples or different types of imaging tests. The risk of relapse decreases with time.
Surgery
The surgery is usually done with a local anesthetic, but the surgery type and extent depends on how the tumor looks. The thinnest tumors are cut at one centimeter margin of healthy tissue. However, if the tumor is thicker and has grown deeper into the skin, it is cut off with a two centimeter margin. To cover large wounds, the surgeon sometimes transplant skin from other parts of the body.
Chemotherapy
If the melanoma has already spread, it can sometimes stopped by cell-inhibiting drugs, known as chemotherapy drugs, which stop the uncontrolled proliferation of cancer cells. Cell Inhibitory drugs have side effects, such as nausea and vomiting. Therefore, it is often a good idea to take medicine for nausea before receiving chemotherapy to reduce or prevent the side effect. Another side effect is that the white blood cells can reduce the number, which means that you can be more susceptible to infections. It is also common to lose your appetite or get dry mouth and diarrhea. If it is difficult to eat or keep food in, you can get in touch with a dietitian. Some cell-inhibiting drugs cause hair loss as well.
Radiation therapy is used in some cases to damage cells in different ways. Some findings prove that cancer cells are sometimes particularly susceptible to radiation therapy. Radiation therapy can cause different types of reactions, depending on what part of the body irradiated, how high radiation doses as the body is exposed to. Some common side effects of radiation therapy include fatigue and skin changes such as redness and irritation. Adverse reactions can be more difficult if you are already weakened by other diseases.
Try our FREE dermatology search engine and get peace of mind within a second
Updated on April 09, 2024
Sources:
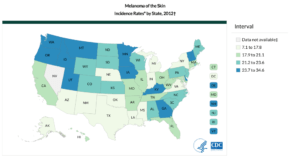
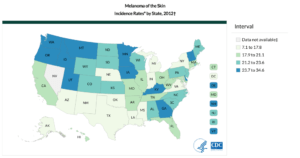
U.S. Cancer Statistics Working Group. United States Cancer Statistics: 1999–2012 Incidence and Mortality Web-based Report. Atlanta: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute; 2015. Available at: https://www.cdc.gov/cancer/dcpc/data/
AIM at Melanoma Foundation. Melanoma Stats, Facts, and Figures. Available at: https://www.aimatmelanoma.org/about-melanoma/melanoma-stats-facts-and-figures/.
American Academy of Dermatology. Melanoma. Available at: https://www.aad.org/public/diseases/skin-cancer/melanoma
National Cancer Institute. SEER Stat Fact Sheets: Melanoma of the Skin. Available at: http://seer.cancer.gov/statfacts/html/melan.html
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.