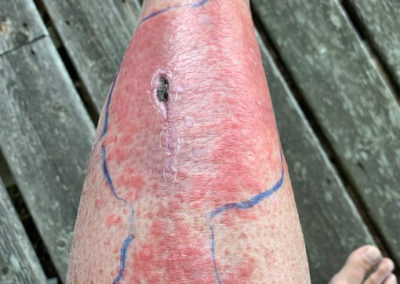
Erysipelas
Medically reviewed by The Dermatologists and written by Dr. Aayushi Shah
Common
- Can lead to severe bacterial infection
- Affecting deeper layers of the skin
- Requires course of antibiotics under medical supervision
- Must seek medical care at the earliest
- Most cases respond well to treatment and heal without scarring
- Risk of recurrences and complications present
Erysipelas is a superficial bacterial infection involving the upper layers of the skin, that is, the dermis and upper subcutaneous tissue. It often involves the lymphatics of the skin. It has a characteristic fiery red appearance along with streaking (due to lymphatic involvement); hence it is also known as “St. Anthony’s Fire”. At times it may overlap with cellulitis, which involves the deeper layers of the skin
Symptoms
Erysipelas often has an acute course. It presents with redness, heat, swelling, pain, and tenderness in the affected areas. There is often an accompanying fever and malaise. It has an acute course, the symptoms can appear overnight and rapidly increase in severity. The onset is often accompanied by severe fever, chills, and rigors.
Classically, the area of involvement in erysipelas is raised above the surrounding skin and inflamed, and there is a distinct demarcation between the involved and normal areas. The lower legs, face, and ears are the most frequently involved regions. There is an accompanying swelling of the lymph nodes in the affected areas. Facial erysipelas are now seen less often, while those affecting extremities remain common. Perianal and periorbital infections can occur rarely.
Erysipelas can occur in children, however, in adults this infection is common in the fourth to sixth decade. Moreover, it can be seen in any age group, especially in patients with predisposing factors. The predisposing factors are the same as those for cellulitis – diabetes, minor cuts or injuries to the skin, insect bites, obesity, immunosuppression, surgical wounds, etc.
In severe and advanced cases of erysipelas, we might note features such as blistering of the skin, necrosis or gangrene (darkening due to dead tissue), and purpura (blood spots).
Bullous erysipelas are the variants of this infection with marked blistering.
Try our FREE dermatology search engine and get peace of mind within a second
What causes it?
Erysipelas can be caused by a variety of bacteria, which can enter the skin through minor cuts or abrasions. Staphylococci and streptococci are two of the common bugs which can cause this infection. Group B streptococci remain the most common cause of infection. Other causes are klebsiella, haemophilus influenzae and pneumococci.
Should I seek medical advice?
Home remedies would not work and are also not advisable since erysipelas can be a severe infection. You must visit the emergency care department or your primary care physician if you suspect that you have this condition, so that antibiotics can be started at the earliest. Early treatment will help a better recovery and reduce the risk of complications and life-threatening septicaemia.
What can I do?
- Leg Elevation
- Cold packs
- Soothing emollients for the skin and antibiotic creams for open sores
- Paracetamol for pain relief
- Rest and lots of fluids
- Seek medical advice
- Control of blood sugars if diabetic
- Compression stockings if marked lower limb swelling
Treatment
Erysipelas can only be treated with a course of antibiotics. Oral antibiotics are needed in most cases, however, advanced cases may also require injectable treatments and hospital admission. Penicillins or tetracyclines are the common antibiotics, however, your doctor may select or change the drug after performing antibiotic sensitivity testing. The antibiotic course usually lasts for 10 to 14 days.
Those with coexisting diseases such as diabetes should seek medical help early. The diagnosis is usually based upon clinical examination, however, blood culture may also be performed to isolate the causative organism.
Blood tests including a complete haemogram to check the white cell count, blood sugar levels, and inflammatory blood markers such as Erythrocyte Sedimentation Rate and C-reactive protein will likely be performed to help plan the treatment.
Outlook
While the systemic symptoms such as fever and chills may resolve within 48 hrs of starting antibiotics, the local signs such as redness and swelling usually resolve over two to four weeks. The skin may take longer to heal completely.
Recurrences do occur, especially in cases with inadequate treatment and persistence of predisposing factors.
Usually, the skin heals without scarring.
Rarely, complications or sequelae such as the infection affecting the heart (endocarditis) or the kidneys (glomerulonephritis) may occur.
Try our FREE dermatology search engine and get peace of mind within a second
Source:
1. Habif, Thomas P. Clinical dermatology. 5th ed. Mosby Elsevier. 2010.
Ask a Dermatologist
Anonymous, fast and secure!

Dr Aayushi Shah is a practising dermatologist from India, currently based in the UK. She has 5 publications has authored chapters covering a wide range of topics, including chronic urticaria, psoriasis, and skin moisturisers. She also works as a Medical Editor, and enjoys blogging in her free time.