Eczema herpeticum
Medically reviewed by The Dermatologists and written by Dr. Alexander Börve
- What It Is: Skin infection marked by fever and clusters of itchy blisters, often complicating atopic dermatitis. Also known as Kaposi varicelliform eruption.
- Causes: Primarily caused by the herpes simplex virus types 1 or 2. It typically occurs during the first exposure to herpes simplex, with signs appearing 5–12 days after contact.
- Who’s at Risk: Affects both genders and all ages, but more common in infants and children with atopic dermatitis. Those with atopic dermatitis have lower resistance to the herpes infection.
- Symptoms and Spread: Starts with painful, itchy blisters on the face and neck, potentially spreading across the body. Accompanied by fever and swollen lymph nodes, blisters may become filled with fluid or pus and can weep, bleed, or form crusts.
Eczema herpeticum, is a severe viral infection that affects individuals with pre-existing skin conditions, particularly atopic dermatitis.This condition, characterized by the rapid spread of herpes simplex virus (HSV) infection across eczematous skin, poses considerable challenges in both diagnosis and management.
While eczema itself presents a host of discomforts and complications, the advent of eczema herpeticum magnifies the complexity of its treatment and demands heightened clinical vigilance.
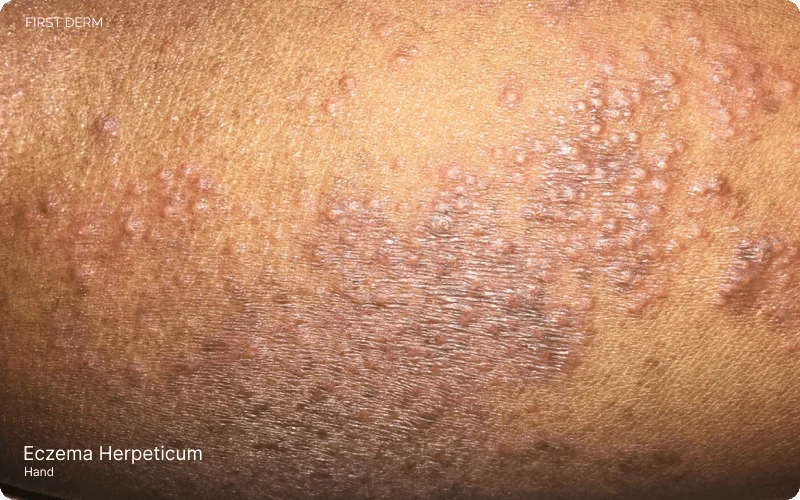
Eczema herpeticum: Atopic dermatitis flare-up with herpes simplex virus infection near elbow
What is Eczema Herpeticum?
Eczema herpeticum, also known as Kaposi varicelliform eruption, is a severe viral infection characterized by the rapid dissemination of herpes simplex virus (HSV) across the eczematous skin.[1] This condition typically manifests as clusters of vesicles or pustules on areas affected by pre-existing dermatoses, most commonly atopic dermatitis (AD).
Eczema Herpeticum: Link Between Atopic Dermatitis and Other Skin Conditions
Atopic Dermatitis (AD)
Eczema herpeticum predominantly affects individuals with pre-existing Atopic Dermatitis, a chronic inflammatory skin disorder characterized by pruritic, erythematous, and eczematous lesions. The disrupted skin barrier in AD facilitates the entry of HSV, predisposing patients to eczema herpeticum. Approximately 10% to 30% of AD patients may experience at least one episode of eczema herpeticum during their lifetime.[2]
Other Skin Conditions
While AD represents the primary predisposing factor, eczema herpeticum can also occur in association with other dermatological conditions, including seborrheic dermatitis, irritant contact dermatitis, and psoriasis. However, the incidence is relatively lower compared to its association with AD.
Eczema Herpeticum: Key Causes and Risk Factors
The Main Triggers of Eczema Herpeticum:
Herpes Simplex Virus Types 1 and 2
- HSV-1 (Herpes Simplex Virus Type 1): Commonly causes cold sores or fever blisters around the mouth. In people with atopic dermatitis, whose skin barrier is weakened, HSV-1 can trigger eczema herpeticum, leading to severe skin infections.
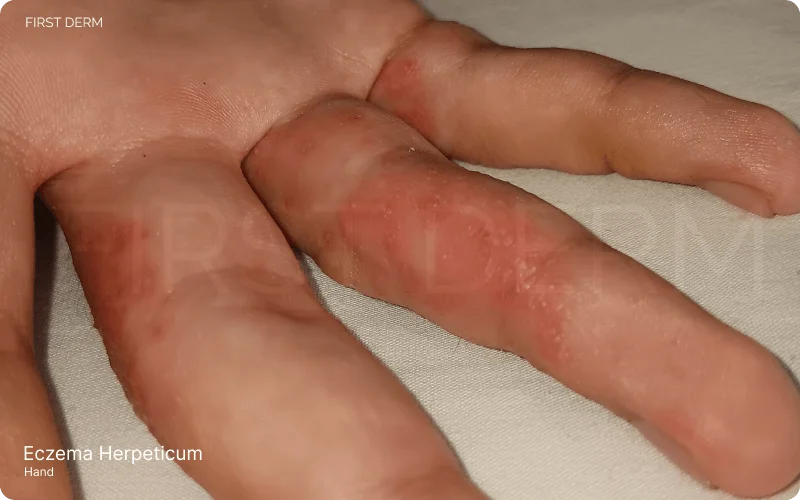
Eczema Herpeticum: A close-up view of cold sores and small blisters on inflamed eczema-affected hands and fingers
- HSV-2 (Herpes Simplex Virus Type 2): Though primarily linked to genital herpes, HSV-2 can also spark eczema herpeticum if it enters the skin of someone with an existing skin condition. The result is often widespread skin lesions and more systemic health issues.
Additional Factors That Increase Risk
- Skin Trauma: Activities that damage the skin, like scratching due to atopic dermatitis itchiness, can make it easier for the herpes virus to cause infections like eczema herpeticum.[3]
- Weakened Immune System: Having a weakened immune system, whether due to certain health conditions or medications, increases vulnerability to aggressive viral infections, including eczema herpeticum.
- Environmental Triggers: Contact with environmental irritants or allergens can worsen atopic dermatitis. This not only aggravates the condition but also may heighten the risk of developing eczema herpeticum.
- Genetic Susceptibility: A person’s genetic makeup can influence their likelihood of developing atopic dermatitis and might affect the severity of skin reactions, potentially increasing the risk of eczema herpeticum.


Why Atopic Dermatitis Increases the Risk of Eczema Herpeticum
Atopic dermatitis, often known as eczema, involves more than just itchy and inflamed skin; it’s also linked to how the body’s immune system works. This connection is crucial for understanding why people with eczema might face a higher risk of developing eczema herpeticum.
Immune System Challenges in Atopic Dermatitis
- T-Cell Dysfunction: In atopic dermatitis, T-cells, which are crucial for immune defense, malfunction. This results in an impaired ability to fight infections effectively, increasing susceptibility to conditions such as eczema herpeticum.[4]
- Cytokine Dysregulation: Atopic dermatitis is characterized by increased levels of pro-inflammatory cytokines, such as interleukin-4 (IL-4), interleukin-5 (IL-5), and interleukin-13 (IL-13). These cytokines contribute to skin barrier dysfunction and impair the immune response to viral infections.
How Immune Dysfunction Affects the Skin
- Weaker Skin Barrier: Atopic dermatitis weakens the skin’s protective layer, largely because the immune system isn’t working properly. This compromised barrier facilitates the entry of viruses, increasing the risk of infections.
- Poor Response to Viruses: With eczema, the body’s usual defenses against viruses are less effective. This means that viruses like the herpes simplex virus, responsible for eczema herpeticum, can cause more severe infections compared to individuals without eczema.
Symptoms and Diagnosis of Eczema Herpeticum
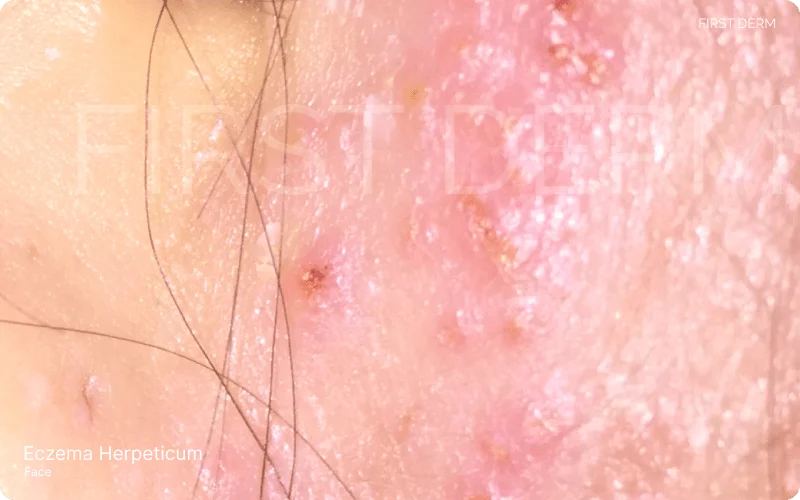
Raised bumps on the jawline, side of the face, and along the ear over a red patch of eczema, indicating eczema herpeticum
- Fever: Patients with eczema herpeticum often present with a high fever, which can be a prominent early sign of the infection.
- Lymphadenopathy: Enlargement of regional lymph nodes, particularly those draining the affected skin areas, is commonly observed in eczema herpeticum. Lymphadenopathy may be tender to palpation and is indicative of the body’s immune response to viral infection.[5]
- Characteristic Skin Lesions: Characteristic skin lesions of eczema herpeticum typically present as vesicular eruptions on the skin , often in areas affected by atopic dermatitis. These clusters of vesicles are filled with clear fluid and can be painful and itchy. Common sites for these characteristic lesions include the face, neck, and areas with pre-existing skin conditions like atopic dermatitis. Identifying these vesicular lesions is crucial in the clinical diagnosis of eczema herpeticum.
Diagnosis of Eczema Herpeticum
Clinical Signs:
- Vesicular Rash: The presence of vesicular lesions, especially in areas affected by atopic dermatitis, is a key clinical sign of eczema herpeticum.
- Erythema and Edema: Redness and swelling around the affected skin, often accompanied by pain and itching, are common clinical features.
- Systemic Symptoms: Patients may exhibit systemic symptoms such as malaise, fatigue, and generalized discomfort.
Step-by-Step Guide:
- Clinical Examination: A thorough physical examination focusing on the skin lesions, lymph nodes, and any systemic symptoms is essential for diagnosing eczema herpeticum.
- Differential Diagnosis: It is crucial to differentiate eczema herpeticum from other skin conditions with similar presentations, such as impetigo or eczema exacerbations.
- Laboratory Tests: Confirmatory laboratory tests, including viral cultures, polymerase chain reaction (PCR) testing for herpes simplex virus, and serological tests, can help in confirming the diagnosis.[6]
- Advancements in Diagnostic Technologies: Recent advancements in diagnostic technologies, such as rapid PCR tests and point-of-care testing, have improved the accuracy and speed of diagnosing eczema herpeticum, enabling prompt initiation of treatment.
Treatment Options for Eczema Herpeticum
Antiviral Treatments:
- Oral Antiviral Medications: Oral antiviral medications, such as acyclovir , valacyclovir, and famciclovir, are commonly prescribed to treat eczema herpeticum.[7] These medications help inhibit the replication of the herpes simplex virus and reduce the severity and duration of the infection.
- Intravenous Antiviral Therapy: In severe cases or when oral medications are not effective, intravenous antiviral therapy may be necessary. Intravenous acyclovir is often used in hospitalized patients with extensive or systemic involvement of eczema herpeticum.
Role of Systemic Antibiotics
- Secondary Bacterial Infections: Systemic antibiotics may be prescribed if secondary bacterial infections complicate eczema herpeticum. These infections can occur due to skin barrier compromise and the presence of open lesions, making antibiotic therapy essential to address bacterial superinfections.
Use of Topical Steroids
- Managing Atopic Dermatitis: Topical steroids play a crucial role in managing underlying atopic dermatitis in the context of eczema herpeticum. While caution is needed due to the risk of exacerbating viral infections, judicious use of topical steroids under medical supervision can help control inflammation and improve skin barrier function in patients with atopic dermatitis.
Complications of Eczema Herpeticum
- Disseminated Infection: Eczema herpeticum can progress to disseminated herpes simplex virus (HSV) infection, spreading to multiple organ systems like the lungs, liver, and central nervous system.[8] This can lead to serious conditions such as pneumonia, hepatitis, and encephalitis.
- Superinfection: Secondary bacterial superinfection is common in eczema herpeticum, especially in cases with extensive skin involvement. Bacteria like Staphylococcus aureus and Streptococcus pyogenes can cause additional infections, requiring prompt antimicrobial treatment.
- Ocular Complications: Involvement of the periocular region in eczema herpeticum can lead to ocular issues like herpetic keratitis, conjunctivitis, and corneal ulcers. Ophthalmologic evaluation and antiviral therapy may be necessary to prevent vision-related complications.
Source
- Wollenberg A, Zoch C, Wetzel S, Gerd Plewig, Przybilla B. Predisposing factors and clinical features of eczema herpeticum: a retrospective analysis of 100 cases. Journal of the American Academy of Dermatology. 2003;49(2):198-205. doi: https://doi.org/10.1067/s0190-9622(03)00896-x
- C Finlow, Thomas J. Disseminated Herpes Simplex Virus: A Case of Eczema Herpeticum Causing Viral Encephalitis. Journal of the Royal College of Physicians of Edinburgh. 2018;48(1):36-39. doi: https://doi.org/10.4997/jrcpe.2018.108
- Damour A, Garcia M, Julien Seneschal, Lévêque N, Bodet C. Eczema Herpeticum: Clinical and Pathophysiological Aspects. Clinical Reviews in Allergy & Immunology. 2019;59(1):1-18. doi: https://doi.org/10.1007/s12016-019-08768-3
- M. Orciani, A. Campanati, M. Caffarini, et al. T helper (Th)1, Th17 and Th2 imbalance in mesenchymal stem cells of adult patients with atopic dermatitis: at the origin of the problem. British Journal of Dermatology. 2017;176(6):1569-1576. doi: https://doi.org/10.1111/bjd.15078
- Xiao A, Tsuchiya A. Eczema Herpeticum. Nih.gov. Published August 8, 2023. Accessed March 15, 2024. https://www.ncbi.nlm.nih.gov/books/NBK560781/
- Frisch S, Siegfried EC. The Clinical Spectrum and Therapeutic Challenge of Eczema Herpeticum. Pediatric Dermatology. 2011;28(1):46-52. doi: https://doi.org/10.1111/j.1525-1470.2010.01356.x
- Niimura M;Nishikawa T. Treatment of eczema herpeticum with oral acyclovir. The American journal of medicine. 2021;85(2A). Accessed March 15, 2024. https://pubmed.ncbi.nlm.nih.gov/3044093/
- Gilles. Visceral Involvement by Herpes Simplex Virus in Eczema Herpeticum. Archives of pediatrics & adolescent medicine. 1968;116(3):324-324. doi: https://doi.org/10.1001/archpedi.1968.02100020326018
- Terezhalmy GT, Tyler MT, Ross GR. Eczema herpeticum: Atopic dermatitis complicated by primary herpetic gingivostomatitis. Oral Surgery, Oral Medicine, Oral Pathology. 1979;48(6):513-516. doi: https://doi.org/10.1016/0030-4220(79)90296-2
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.

