Atypical moles
Medically reviewed by The Dermatologists and written by Dr. Alexander Börve
- Prevalence and Identification: Atypical moles, present in 10% of Americans, are larger, with irregular, notched borders and color variations.
-
Melanoma Risk: Atypical moles increase melanoma risk, especially in individuals with fair skin and heavy freckling, though not all atypical moles become cancerous.
- Risk Factors and Family History: Having more than 10 atypical moles raises melanoma risk 14-fold, with significant risk also in those with a family history of melanoma.
- Diagnosis and Management: A biopsy is essential for diagnosing atypical moles, with severe dysplastic moles typically recommended for removal.
- Self-Examination and Monitoring: Monthly self-examination of skin and annual eye exams are crucial for early detection of melanoma in individuals with atypical moles.
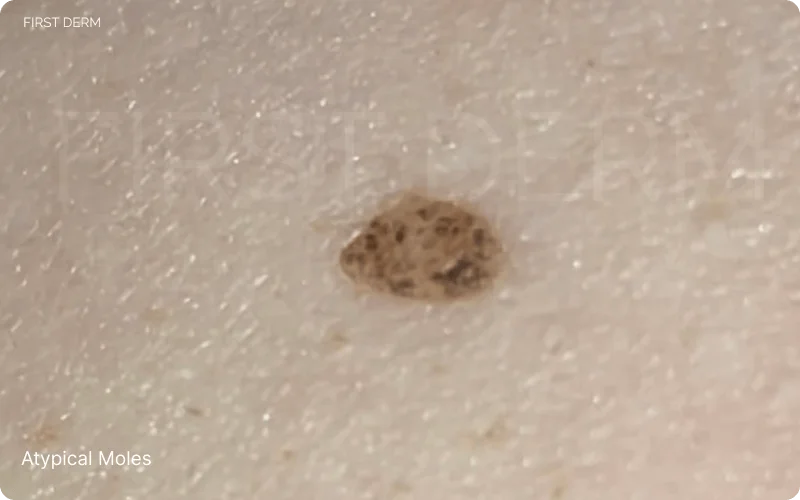
Atypical Nevus, revealing its distinct features: irregular border and color variation, and appearing larger than other moles
Ever noticed a mole that looks peculiar and out of the ordinary? Atypical moles are not just everyday blemishes; they are irregular skin growths that stand out from typical moles due to their distinct features like uneven borders, varied coloration, and larger size.
They also signify potential risks. One such dangerous outcome is conversion into malignant melanoma, which is a skin cancer that spreads very quickly.
What are atypical moles?
Atypical moles are now known by various other names, including dysplastic nevi, BK moles, Clark nevi and nevi with architectural disorder.[2]
It is recognised as an intermediary stage between harmless moles and melanoma, featuring junctional melanocytic skin lesions (lesion at the junction between dermal and epidermal layers of the skin) displaying abnormal changes.[1]
Sometimes, clinical features may lead to confusion because atypical moles are significantly similar to melanoma in appearance to the naked eye. As a solution to this problem, Stolz et al. proposed the “ABCDE” rule and the total dermoscopy score (TDS) derived from it as a helpful way to distinguish melanoma from common moles during diagnosis.[3]
Identifying Atypical Moles
ABCDE method contains several criteria including asymmetry, border irregularity, color variation, larger diameter and evolving changes in size, shape, or color. These moles are frequently characterized as pigmented skin lesions that develop spontaneously or are inherited, exhibiting clinical and histological features distinct from typical moles.
They tend to be larger in size, often exceeding 5 mm in diameter, and display varied colors ranging from tan to dark brown, sometimes accompanied by a reddish background that fades under pressure.[2] These nevi can present as flat macules or raised papules, with irregular and poorly defined borders. While they can appear anywhere on the body, they are commonly found on the trunk. Unlike typical moles that emerge in childhood, atypical nevi typically arise around puberty and evolve throughout adulthood. But they rarely appear after the age of 60.[2]
Clinical subtypes of atypical moles
Atypical moles manifest in five distinct clinical subtypes[1]
- Fried-egg subtype: featuring a raised central portion with dark brown pigmentation, encircled by a lighter brown, poorly defined area.
- Lentiginous subtype: presenting a uniformly flat surface with brown or dark brown pigmentation.
- Seborrheic keratosis-like subtype: displaying dark brown pigmentation and a rough, warty surface akin to seborrheic keratosis.
- Targeted subtype: characterized by a central annular zone with varying pigmentation.
- Erythematous subtype: recognizable by its pink pigmentation and minimal pigmentation remnants.
Risk Factors and Prevalence
Both genetic factors and exposure to ultraviolet (UV) radiation are believed to contribute to the formation of atypical moles. Therefore, people with risk factors such as fair skin type, family history, and excessive sun exposure are more at risk. Individuals of Caucasian descent, particularly those with fair skin like Celtic people, are more susceptible to developing numerous atypical moles, whereas this condition is uncommon among other ethnicities.[4] Atypical nevi can develop by chance (sporadically) or be inherited within families, leading to sporadic and familial types.
Atypical Mole Syndrome and Familial Atypical Multiple Mole Melanoma Syndrome (FAMMM) denote conditions where individuals have more than 50 pigmented nevi, among which, at least 3 show atypical features mentioned above.[4] They also have one or more close relatives who is diagnosed with melanoma.
According to K. E. Wensley and P. M. Zito, while the lifetime risk of melanoma for the general population in the United States remains below 1%, it dramatically surpasses 10% for individuals with atypical moles.[1] Risk of malignant conversion of atypical moles in one’s lifetime in FAMMM is known to be close to 100%, highlighting the importance of vigilant monitoring and early detection.[1]


What causes atypical moles
A combination of internal genetic factors, host factors and external environmental factors contribute to the formation of atypical moles. They often appear in individuals with fair skin, light hair and eye color, freckles, and sensitivity to sunlight. Studies link specific genetic markers like IRF4, PLA2G6, and MTAP to their occurrence.[1]
Managing and Monitoring Atypical Moles
The first step in managing atypical moles is careful self-examination and monitoring. This helps you identify atypical moles, and track whether there are any changes in size and colour. Studies have shown increased number of moles itself is a risk factor for melanoma, and they further stated correct identification of dysplastic ones help predict the level of risk more accurately.[5]
Total body photographing is a recommended method to keep track of these changes over time.[5] Regular visits to your healthcare provider is encouraged if you have a lot of moles. This is because of two reasons. First is, you are likely to miss some moles in self-examination, so the trained clinician’s count is usually greater than that of your own. The second reason is clinicians can use dermoscopic examination of the moles to see the changes that might not be visible to the naked eye. Moles are again subdivided as Reticular, Globular, Homogeneous, Reticular-globular, Reticular-homogeneous and Globular-homogeneous, depending on the dermoscopic appearance.[3] How often you must make these doctor visits depend on your age, gender and the changes observed in the moles.[5]
However, most reliable way of diagnosis and risk prediction is histology, where a piece of tissue will be examined under a microscope.[1] This is accomplished by taking a biopsy, which most of the time will remove the entire mole from the skin (excision biopsy method). Managing the lesion after the biopsy can be variable. According to a survey done by the American Academy of Dermatology, over half of doctors stated that they re-excise atypical moles if margins are incomplete or if lesions come back.[1] This is because if a lesion grows back along a scar, it might look like melanoma, a phenomenon called ‘pseudo-melanoma’.
But newer evidence supports that careful observation of these excised moles can give you similar results to re-excision.[2]
Removing all the moles as a preventive method is not recommended because of two reasons. Not all moles turn into melanoma, it is only a significant minority. Also, only 20% melanomas arise from atypical moles, which means most melanoma arise de novo, so your risk of getting melanoma is not zeroed just because you removed all the moles.[5]
Treatment and Prevention
Moles may need removal if they show concerning changes or exhibit features suggesting melanoma. Such instances include when there’s doubt about whether the clinical exam matches the tissue analysis, severe abnormality, or if the tissue can’t be clearly identified from melanoma. The mole should be managed like melanoma according to guidelines: it should be removed with proper margins.
Excision biopsy (removing the entire lesion) is the recommended method over incision biopsy (cutting out a part of the lesion).[1] Even though there is no known way to prevent occurrence of atypical moles completely, protecting skin from sun damage plays a role in lowering the risk.[1] Sun protection tips include wearing sunscreen with a high spf value (50+), seeking shade, and wearing protective clothing. Regular skin checks help monitor changes in moles and detect any potential issues early.
Living with Atypical Moles
As discussed above, despite the significant potential risk of converting to melanoma, most of the atypical nevi do not. They either remain unchanged or regress. Therefore, you do not need to get depressed about having atypical moles, as long as you monitor them carefully in the described manner. Do not forget to document the variations you note using photography method, and consult your health care provider regularly. It is important to educate family members about melanoma risk and prevention measures, such as sun protection and regular skin checks, to promote early detection and proactive health management.
Conclusion
In conclusion, the significance of recognizing atypical moles cannot be overstated. These quirky skin marks serve as potential indicators of melanoma risk, making awareness crucial for early detection and treatment. By staying vigilant and regularly checking your skin, you can take proactive steps in safeguarding your skin health. Remember, knowledge is power, and with it, we can embrace a future of melanoma prevention and overall well-being.
Source
- Wensley KE, Zito PM. Atypical mole. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK560606. Published July 3, 2023.
- Kmetz EC, Sanders H, Fisher G, Lang PG, Maize JC Sr. The role of observation in the management of atypical nevi. South Med J. 2009;102(1):45-48. doi:10.1097/SMJ.0b013e3181904289
- Suh KS, Park JB, Kim JH, et al. Dysplastic nevus : Clinical features and usefulness of dermoscopy. J Dermatol. 2019;46(2):e76-e77. doi:10.1111/1346-8138.14583
- British Association of Dermatologists. www.bad.org.uk. Published January 2020. Accessed March 29, 2024. https://www.bad.org.uk/pils/atypical-mole-syndrome/
- Goldstein AM, Tucker MA. Dysplastic nevi and melanoma. Cancer Epidemiol Biomarkers Prev. 2013;22(4):528-532. doi:10.1158/1055-9965.EPI-12-1346
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.

