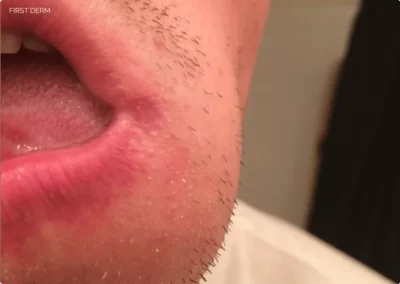
Angular cheilitis
- Affects about 0.7% of the general American population, with a higher incidence among the elderly (11%) and denture wearers (28%)
- Cause cracks, sores, and inflammation at the corners of the mouth
- Common cause: Excessive saliva exposure leading to skin damage and infection
- Other causes: Atopic dermatitis, long-term use of certain medications, nutritional deficiencies, and chronic illnesses like diabetes and inflammatory bowel disease
- Condition’s severity: Mild redness to severe, potentially bleeding cracks and crusting
- More prevalent in children, the elderly, and denture wearers.
- Diagnosis: Typically based on clinical history and physical examination
- ICD: K13.0
Angular cheilitis, a common yet troublesome visitor, can be a real inconvenience, giving rise to cracks, sores, and inflammation at the corners of your mouth. Not only does it mar your appearance, but it can also disrupt normal activities like eating and speaking. Understanding the causes, symptoms, and treatments for this condition is key to regaining comfort and confidence in your smile.
Often known by other names like angular cheilosis, angular stomatitis, commissural stomatitis, rhagades, or perleche, this condition affects around 0.7% of the general American population.1 However, it is not evenly distributed across all age groups. Children are more prone to angular cheilitis, and its incidence is markedly higher among the elderly population at 11%. In fact, it’s observed three-fold more among those who wear dentures, with the likelihood going up to as high as 28%.1
The occurrence of angular cheilitis shows no gender preference according to studies. Good oral hygiene, though, has been found to significantly reduce its occurrence.2 The term ‘Perleche’ comes from the French term meaning “through licking”, and ‘rhagades’ refers to cracks or fissures in skin areas subject to frequent movement, such as the corners of the mouth (labial commissures) or the nose. These terms aptly illustrate the very mechanisms behind the development of angular cheilitis.
Despite the varying causes, ranging from dryness and nutritional deficiencies to fungal or bacterial infections and ill-fitting dentures, there are effective treatments available. In the following sections, we will delve deeper into the aspects of this condition, empowering you with the knowledge to combat this pesky visitor and reclaim your smile.
Causes
The main cause in most cases is excessive exposure to saliva, which leads to the softening and damage of the skin at the corners of the mouth. Upon prolonged exposure, the digestive enzymes present in saliva can act on the skin and cause inflammation, giving the perfect opportunity for different microorganisms which are normally present on the skin to infect the area. These microorganisms include fungi like Candida albicans and bacteria like Streptococcus and Staphylococcus species.
Apart from this most common reason, other factors like atopic dermatitis, Sjogres syndrome, and recurrent chemical, thermal or mechanical injury can be the cause behind it.
Therefore, if you have a habit of thumb-sucking, eating lollipops, aggressive dental flossing, smoking or nervous tics such as over-licking your lips, you are more at risk to suffer from this.
Long-term use of medications like antibiotics and immunosuppressants is another cause.
Even though less common, some nutritional deficiencies like vitamin B2, B9, B12, trace minerals (iron or zinc), and general protein malnutrition can also be the underlying cause. 3
Certain long-standing illnesses such as diabetes mellitus, inflammatory bowel disease or Down syndrome are other known causes.
Identification of Angular Cheilitis
General Appearance:
When you look at the area it will appear red and swollen. These inflamed patches of skin are roughly triangular in shape.
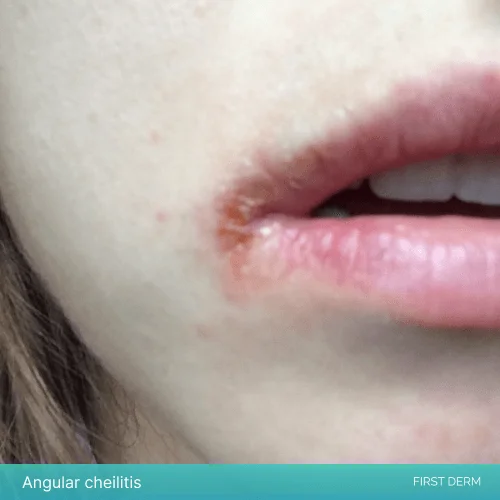
Visual representation of Angular Cheilitis: Notice the inflamed patches at the corners of the mouth, a key identifier of this common skin condition
Mild Cases:
When it is mild, there might not be any change in appearance except for some pinkish erythema with normal-looking or chapped lips. As the condition progresses, the presence of moisture causes the outer layer of the skin to soften and wear away, resulting in small grey-white sores surrounded by red tissue at the corners of the mouth.
Moderate Cases:
In moderate cases, the affected skin becomes raised, inflamed, and more cracked. These well-established sores may appear bluish-white with flaky skin accompanied by redness.
Severe Cases:
Severe cases can cause deep cracks that may bleed, although this is uncommon in angular cheilitis. In cases of significant inflammation, damaged skin can release fluids and form crusts, but this is more commonly seen in the later stages of the condition.
Additional Observations:
Bacterial angular cheilitis is more likely to exhibit yellowish-coloured fluid, pus-filled bumps, and purulent discharge. Rarely, leukoplakia (thick, white patches on the mucous membranes of the mouth) may be observed.
Location:
Also, it is present in both corners usually, unless there is a specific reason for exposing only one side to the risk factors mentioned above.
Clinical Stages:
Clinically, 4 stages are identified. The most common is stage 1, where the lesion is limited to the corner of the mouth and the surrounding skin is slightly folded inward. 4
Diagnosis of Angular Cheilitis
General Approach
Your doctor will be able to make the diagnosis based purely on history and the clinical picture. Usually, laboratory tests are not performed.
In Case of Treatment Failure
However, if initial treatment fails, it is advisable to go for laboratory investigations. These investigations vary on the suspected cause of the angular cheilitis.
Testing for Infections
Since infection is the most common cause, first tests are carried out to see if there are any fungi or bacteria present. Tests for common fungal infection with Candida include light microscopy, germ tube tests, sugar assimilation assays, fungal culture, Candida strain typing and immunodiagnosis (Eg. ELISA).1 To detect bacteria, bacterial cultures are done.
Assessing Nutritional Deficiencies
Nutritional deficiencies can be assessed with simple blood and urine tests, including serum folic acid levels, serum vitamin B12 levels, serum iron profile, serum zinc level and urinary riboflavin excretion tests.
Detecting Allergic or Irritant Conditions
If allergic or irritant conditions are suspected, a patch test is done to determine if there is any allergic contact dermatitis.
More than 70% of our users get better with Over-the-Counter Medication
Treatment of Angular Cheilitis
General Approach
Even though it can cause major inconvenience and discomfort, angular cheilitis is not a serious or life-threatening disease. Much like the diagnostic tests, the treatment also differs according to the cause. It typically involves addressing the underlying causes and promoting the healing of the affected skin.
First-Line Treatment
First-line treatment includes antifungals and antibacterials. If a fungal or bacterial infection is present, topical antifungal or antibacterial creams may be prescribed to combat the infection and promote healing. Nystatin, Gentian, Ketoconazole and Miconazole are common antifungals, which are topically applied 3 times a day for 2 weeks. Antibacterials include Mupirocin and Fusidic acid.
Oral Medications
Oral medication is there as well, which will be prescribed by your medical health professional if the lesions are extensive or when the initial treatment fails.
Inflammatory Cases:
In cases of significant inflammation, topical corticosteroid creams or ointments may be used to reduce swelling, redness, and discomfort. It might be used together with antifungal or antibacterial medication to give you relief from the symptoms.
Ill-Fitting Dentures:
If the condition is caused or worsened by ill-fitting dentures, adjusting or replacing them can provide relief and aid in healing.
Nutritional Deficiencies:
In instances where angular cheilitis is associated with nutritional deficiencies, such as deficiencies in iron, vitamin B12, or zinc, taking appropriate nutritional supplements can help address these deficiencies.
Treatment Failure and Complications
Reasons for Failure
If treatment fails, it can be due to various reasons. Some common ones are not recognizing or treating oral candidiasis properly, which can worsen the condition. In some cases, certain types of Candida or bacteria may be resistant to treatment, making it harder to get results. Not addressing things like poor oral hygiene, poorly fitting dentures, or specific habits can also make healing difficult. Other factors like persistent risks, nutritional deficiencies, inflammatory conditions, and suppressed immune system, can all contribute to treatment failures. It’s important to address these factors thoroughly to improve treatment effectiveness and achieve successful outcomes.
Complications:
Complications when long-standing include lasting tissue damage, including atrophy (cell death), permanent scarring, or discolouration.
Prevention of Angular Cheilitis
Maintain Oral Hygiene
Keep those mouth corners clean to prevent excessive moisture buildup. Practice good oral hygiene: Brush your teeth twice a day and floss daily. This helps reduce the accumulation of bacteria around the mouth corners.
Avoid Certain Habits
Excessive licking of the lips can lead to further moisture and irritation, making the condition worse. Try to avoid the habits of lip licking and tobacco smoking.
Keep Lips Hydrated
Apply a lip balm or moisturizing ointment to keep your lips well-hydrated and prevent dryness or cracking.
Protect Your Lips
Protect your lips from extreme weather conditions. In cold or windy weather, use a scarf or a lip balm with SPF to protect your lips from drying out.
Manage Underlying Health Issues
Certain medical conditions like vitamin deficiencies, yeast infections, or hormonal imbalances can contribute to angular cheilitis. If you have any underlying health issues, work with your healthcare provider to manage them effectively.
Balanced Diet
A nutritious and balanced diet is important to avoid nutritional deficiencies.
Avoid Potential Irritants: Stay away from potential irritants such as harsh cosmetics, fragrances, or lip products that may cause allergic reactions or dryness.
Proper Denture Care
If you wear dentures, clean and maintain them properly to prevent irritation. Discard ill-fitting dentures that can contribute to angular cheilitis and go for a proper fit.
FAQ
Is angular cheilitis an STI?
No, angular cheilitis is not a sexually transmitted infection (STI). It is typically caused by factors like excessive or prolonged saliva exposure, fungal or bacterial infections, or underlying health conditions.
How long does angular cheilitis take to heal?
The healing time for angular cheilitis can differ depending on the underlying causative factor. Mild cases may resolve within a few days to a couple of weeks with proper treatment.
Can angular cheilitis recur?
Yes, angular cheilitis can recur, especially if the causes or risk factors are not properly addressed or managed.
What worsens Angular Cheilitis?
Factors that can worsen angular cheilitis include excessive saliva exposure/accumulation, licking the lips, poor oral hygiene, nutritional deficiencies, and untreated fungal or bacterial infections.
What happens if Angular Cheilitis is left untreated?
Untreated angular cheilitis can lead to persistent symptoms, worsening pain, increased risk of infection, and possible scarring or discolouration of the affected area.
Can Angular Cheilitis be a sign of an underlying health condition?
Yes, in some cases, angular cheilitis can be linked to underlying health conditions such as nutritional deficiencies, autoimmune disorders, or systemic diseases. It is important to consult a healthcare professional for proper evaluation and management.
Should I let Angular Cheilitis dry out?
It is generally recommended to keep the affected area clean and moisturized rather than letting it excessively dry out. Moisturizing helps prevent further cracking and discomfort.
What is the quickest home remedy for Angular Cheilitis?
Applying a protective lip balm or ointment, keeping the area clean and dry, and addressing underlying causes such as nutritional deficiencies are some home remedies that may help alleviate angular cheilitis.
Can Cheilitis be a result of Covid?
There is no direct evidence linking cheilitis to Covid-19. However, Covid-19 can cause various oral symptoms, and cheilitis could potentially occur as a secondary effect in some cases.
Can you kiss with Angular Cheilitis?
It is generally advisable to avoid intimate contact or kissing until the angular cheilitis has fully healed to prevent the potential transmission of any infectious agents or discomfort to the affected area.
Reference
- Federico, J. R., Basehore, B. M., & Zito, P. M. (2023). Angular Chelitis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK536929/
- Cross, D., Eide, M. L., & Kotinas, A. (2010). The clinical features of angular cheilitis occurring during orthodontic treatment: a multi-centre observational study. Journal of Orthodontics, 37(2), 80–86. https://doi.org/10.1016/S0140-6736(71)92626-2
- Oza, N., & Doshi, J. (2017). Angular cheilitis: A clinical and microbial study. Indian Journal of Dental Research : Official Publication of Indian Society for Dental Research, 28(6), 661–665.

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.