Tinea infections
Medically reviewed by The Dermatologists and written by Dr. Aayushi Shah
Common Very common
- Very common skin infection.
- Contagious, spreads through direct contact.
- Requires medical diagnosis and treatment.
- Therapy consists of oral and topical treatments.
- Usually completely curable.
Fungi are ubiquitous organisms, commonly present in almost every environment, and capable of colonizing the skin under favorable conditions. The ringworm type of fungal infections, also called Tinea infections, are a specific type of superficial fungal disease, caused by a group of fungi called Dermatophytes.
Dermatophytes are capable of infecting only the superficial skin layer composed of dead tissue (keratin). This keratin layer is present in the hair, skin, and nails; thus, ringworm infections can occur in all these body parts.
Fungal infections may be acquired by contact with other infected persons, infected pets, or rarely even through contact with soil carrying such fungi.
Symptoms
The dermatophytes, or ringworm fungi, produce a variety of different disease patterns, which have been named according to the body part affected and the type of fungus causing the disease. Tinea infections can occur in children as well as adults, although scalp infections are seen only in children. Certain occupations or contact sports may predispose to such infections, such as wrestling, or being an athlete.
The following is a small list of some of the common types of tinea infections one might come across:
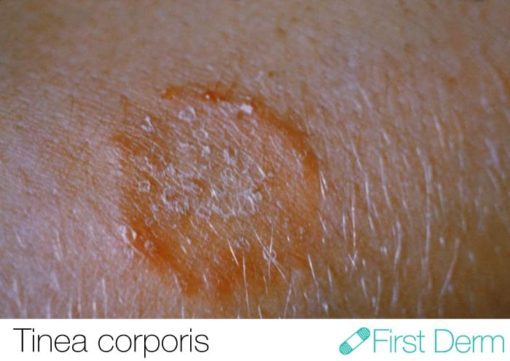
- Tinea corporis: Ringworm infection affecting skin of the trunk or limbs.
- Tinea cruris: Affects skin of the groin.
- Tinea capitis: Ringworm of the scalp, often invades the hair shafts.
- Tinea barbae: Ringworm of the beard and mustache areas with invasion of coarse hair.
- Tinea faciei: Infection involving skin of the face.
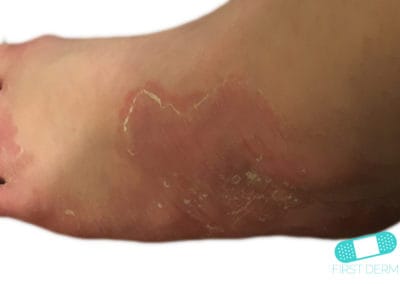
- Tinea pedis: (Athlete’s foot): Ringworm of the foot.
- Tinea manuum: Ringworm of the hand.
- Tinea unguium/ onychomycosis: Ringworm of the nails.
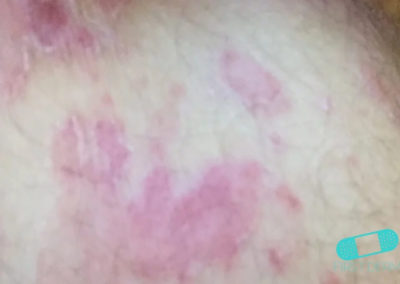
Ringworm is characterised by coin shaped or ring like lesions with a raised border, which might expand at varying rates in all directions. There may be scaling or itching accompanying them. As the rings grow in size, the central area may start to clear out, thus contributing to the characteristic appearance. The rings may occur in any size, either single or multiple, and can be seen over any body part.
Tinea affecting the palms and soles may lead to dry, diffusely thickened, and flaky skin. Itching is uncommon, but may be seen at times. It may also cause yellowish discolouration and thickening of the nails of the hands and feet.
Tinea of the scalp most commonly occurs in children between 3 to 7 years of age. It can be highly infectious due to spread via fungal spores. It can cause a variety of symptoms such as loss of hair, graying of hair shafts, breakage of hair shafts, and boggy red swelling in the scalp.
Tinea incognito is a special name for tinea infections, where the typical appearance of the rash has changed due to application of topical steroids. This can occur due to improper diagnosis or incorrect treatment of the initial rash.
What can I do?
Like all fungal infections, the ringworm infection thrives in a moist environment. Keeping the area clean and dry, and avoiding activities which involve sweating will lead to faster healing. In addition, using over the counter antifungal creams such as clotrimazole, or terbinafine, may cure the infection. Medicated antifungal shampoos may be useful for scalp infections (eg. Nizoral shampoo).
In case of infections of the hands and feet, avoid repeated handwashing and wearing closed footwear. Avoid direct contact with others and sharing of razors, soaps, towels etc. to stop further spread of the disease.
Should I seek medical advice?
If you are unsure of your condition, it is best to seek medical advice, as Tinea infections tend to last long when left untreated. In case of extensive lesions, or any painful inflamed spots, or large sized rings, oral antifungal tablets may be needed to ensure complete cure and avoid recurrences. In case of any scalp or nail infections, it is best to seek medical advice as these can be difficult to treat.
Treatment
- Tinea infections are completely treatable and respond well to medical treatment.
- The treatment is a combination of personal hygiene measures and medical treatment.
- Some fungicidal creams may be given, which need to be applied twice daily, with or without oral fungicidal tablets. The treatment may run for 2-4 weeks, or longer, depending on the severity of infection and the response to treatment.
- Tinea involving the hands, feet, or nails may require prolonged courses of therapy.
- Oral antifungals such as griseofulvin or terbinafine tablets may be used.
- Creams may be either clotrimazole, terbinafine, or miconazole, amongst others.
- Antifungal dusting powders may be used at times, to maintain a dry environment and avoid recurrences.
Source:
1. Habif, Thomas P. Clinical dermatology. 5th ed. Mosby Elsevier. 2010.
Ask a Dermatologist
Anonymous, fast and secure!

Dr Aayushi Shah is a practising dermatologist from India, currently based in the UK. She has 5 publications has authored chapters covering a wide range of topics, including chronic urticaria, psoriasis, and skin moisturisers. She also works as a Medical Editor, and enjoys blogging in her free time.