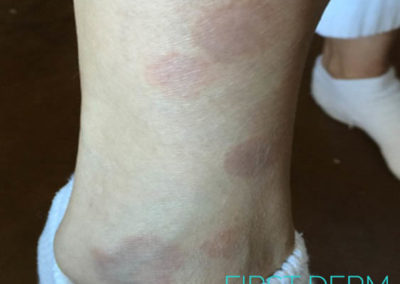
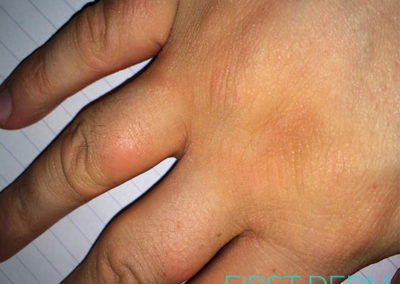
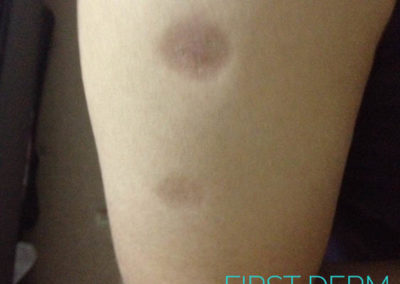
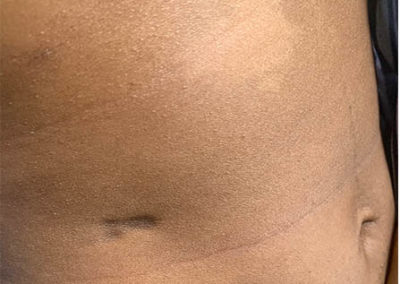
Scleroderma
Medically reviewed by The Dermatologists and written by Dr. Carol Mastropierro and Dr. Alexander Börve
Uncommon
- It can present as mild disease, known as localized scleroderma or extensive disease, known as generalized scleroderma
- Scleroderma is an autoimmune response, leading to overproduction of collagen by cells in the connective tissue. This causes scarring and thickening (fibrosis)
- Treatment is only symptomatic and aimed to prevent the condition getting worse
Scleroderma is an uncommon condition that results in hard, thickened areas of skin and sometimes problems with internal organs and blood vessels.
Scleroderma is caused by the immune system attacking the connective tissue under the skin and around internal organs and blood vessels. This causes scarring and thickening of the tissue in these areas. The pathophysiology behind this autoimmune reaction is not completely understood. However, certain genes are thought to be involved, and having a close family member with the condition may increase your risk, suggesting a degree of inheritance.
Consult an online dermatologist today and get an answer on your skin concern within hours.
Symptoms
The symptoms of scleroderma depend on the severity of the disease. There are two main types of scleroderma:
1. Localised scleroderma – This condition is the mildest as it just affects the skin. It usually presents during childhood but may occur at any age. This type presents with single or multiple patches on the skin. Internal organs are spared. The way the skin is affected by scleroderma is classified as Morphea or linear involment. Morphea is a discolored and itchy patch of skin, which can appear anywhere on the body.
The affected area is often shiny and glabrous (hairless). Morphea lesions may improve after a few years and often do not require treatment. Linear type of involvement presents as a thickened patch of skin occurring along lines and folds of the face, scalp, or limbs. This represents a more severe disease, as it is often accompanied by growth problems, such as shortened limbs.
Consult an online dermatologist today and get an answer on your skin concern within hours.
2. Systemic sclerosis – this condition is the most severe since it may affect blood circulation and internal organs as well as the skin. This type mostly affects women and usually develops between 30 and 50 years of age. Systemic sclerosis can be further divided in two types: limited cutaneous systemic sclerosis and diffuse systemic sclerosis.
3. Limited cutaneous systemic sclerosis is a milder form whose typical symptoms are thickening of the skin of the hands, feet and face. Red spots on the skin and hard lumps under the skin often accompany heartburn and dysphagia. This type of scleroderma frequently presents as Raynaud’s phenomenon. Limited cutaneous systemic sclerosis tends to worsen with aging, but it is well controlled by treatment.
Diffuse systemic sclerosis is the most severe type, as it extensively affects the skin over the whole body and internal organs, especially fibrosis of heart, lungs and kidneys. This results in a a presentation ranging from shortness of breath to high blood pressure or pulmonay hypertension. Symptoms appear suddenly and get worse quickly over the first few years, but the condition normally settles and the skin may gradually improve.
Consult an online dermatologist today and get an answer on your skin concern within hours.
What can I do?
Scleroderma cannot be treated, there are plenty of therapies and lifestyle changes that can help reduce the symptoms and the impact of the disease on your life. It is important for you to eat healthily, exercise regularly and quit smoking. This will help you controlling your blood pressure, which is the most common systemic complications of scleroderma. Furthermore, you should regularly stretch in order to keep your muscles and skin elastic. You will also need to regularly check your blood pressure.
Consult an online dermatologist today and get an answer on your skin concern within hours.
Treatment
There is no cure for scleroderma. The aim of treatment is to relieve symptoms, tackle complications and prevent the disease from getting worse. Common treatment options include medications aimed to control blood pressure and aid circulation, such as ACEi or Calcium Channel Blockers. Considered the autoimmune etiology if this condition, immunosuppressors and steroids are considered in severe and systemic involvement.
Skin thickening is addressed with rich moisturizing agents, in order to keep the affected areas elastic and reduce the itchiness. If you have hard lumps under the skin, those may need to be surgically removed. and tightened muscles may need to be loosened.
Newer treatments involve the use of laser therapy and photodynamic therapy. These are currently being trialed.
Consult an online dermatologist today and get an answer on your skin concern within hours.
Source:
American College of Rheumatology Committee: https://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Scleroderma
The Genetics Home Reference: https://ghr.nlm.nih.gov/condition/systemic-scleroderma
Odonwodo A, Badri T, Hariz A. Scleroderma (Systemic Sclerosis) [Updated 2020 May 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537335/
Adnan ZA. Diagnosis and treatment of scleroderma. Acta Med Indones. 2008;40(2):109-112. https://pubmed.ncbi.nlm.nih.gov/18560030/
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.